Trump cuts HIV funding: treatment held, prevention faltered—new data shows
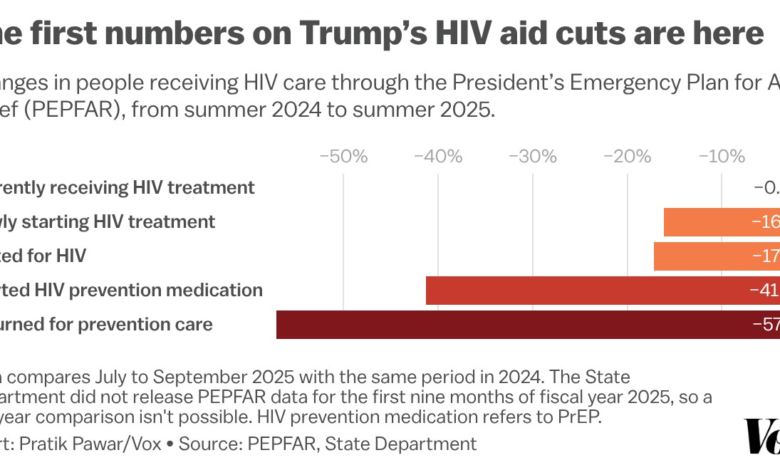
PEPFAR treatment – Official figures suggest PEPFAR kept antiretroviral treatment steady in late 2025, while testing, PrEP and prevention programs sharply declined after the foreign aid freeze.
When the Trump administration began reshaping foreign aid in early 2025, HIV program experts warned the fallout could be severe—especially for prevention work that depends on constant outreach.
The latest official data offers a complicated snapshot of what happened after the cuts.. For the period the government chose to release—July through September 2025—the United States still delivered antiretroviral drugs to about 20 million people.. That continuity in treatment is a real public-health win. and it aligns with the administration’s message that core care was preserved.
But the picture changes when you look beyond the headline number.. HIV programs are not only about keeping people already diagnosed alive; they are also about finding people who don’t know their status and interrupting new infections before they take hold.. In the same released quarter. fewer people were tested for HIV than the year before. fewer people started treatment after diagnosis. and PrEP enrollment—the daily medication that can prevent HIV—dropped dramatically.
This is where the story turns from reassurance to concern.. PEPFAR has long been more than a drug delivery system.. It was built to support an entire prevention-to-care pathway—testing. linkage to treatment. follow-up. and community outreach—because HIV control depends on catching infections early and reaching people who are most at risk.. When that pipeline weakens, the consequences can be delayed but profound.
In the latest quarter of fiscal 2025 that officials released. HIV testing fell by about 17 percent compared with the same time the year before. with roughly 4 million fewer people tested.. The number of people newly starting HIV treatment declined by 16 percent, dropping from about 463,000 to about 389,000.. PrEP—critical for preventing infections among people at higher risk—saw an even larger contraction: new enrollments fell by about 270. 000. a 41 percent drop. and fewer people returned for follow-up. nearly 60 percent fewer than the year before.
There’s also the question of what the released quarter can and cannot tell the public.. The government did not release data for the rest of fiscal 2025, citing reporting and implementation challenges.. According to an analysis that reviewed an earlier set of unpublished figures that appeared briefly online before being removed. the disruptions may have been more extreme across the overall HIV response. with only partial recovery later in the year.. That means even if late-2025 treatment numbers look steadier, other parts of the response may have suffered more sharply.
For people living with HIV, uninterrupted treatment can be the difference between health stability and deterioration.. But for communities trying to avoid infection in the first place. prevention work often depends on flexible staffing and day-to-day trust-building—testing drives. outreach. case management. and follow-up.. Those functions are typically more fragile than the supply chain for medications.. If outreach and prevention staffing thin out. people can simply fall out of the system without a clear immediate signal in treatment-only metrics.
One reason these distinctions matter is that “continuity of care” and “epidemic control” are not identical goals.. Keeping someone on antiretrovirals is crucial; it prevents disease progression and reduces transmission risk.. Yet preventing new infections requires consistent engagement with people who may not routinely access health care. including individuals in key populations and their partners.. The newest data suggests PEPFAR’s prevention footprint shrank at the same time treatment continuity remained relatively intact.
This shift also clashes with the way the HIV epidemic looks today.. Globally, new infections are concentrated among specific groups, and prevention strategies have had to adapt accordingly.. The administration has emphasized mother-to-child transmission prevention and keeping treatment steady. and there is evidence that testing for pregnant women at first prenatal visits increased.. Still. experts argue that focusing too narrowly on pregnancy-related prevention doesn’t match the broader reality of where new infections occur—especially among adolescent girls and young women. and among other groups facing disproportionate risk.
Programs designed for those higher-risk communities appear to have borne some of the brunt of the disruption.. The DREAMS initiative—created to help adolescent girls and young women remain HIV-negative—had nearly 2 million participants in the last quarter of 2024. but that number fell to about 253. 000 a year later.. Prevention programs for key populations also declined sharply. including reports that some prevention participation effectively dropped to zero in the later period.. Taken together. those changes suggest that the system that identifies risk and delivers prevention support weakened. even while treatment coverage stayed closer to baseline.
The administration’s interest in next-generation prevention options adds another layer of urgency.. A longer-acting injectable medicine has been positioned as a major advancement in HIV prevention.. But delivering that kind of tool at scale requires the same kinds of outreach. patient navigation. and follow-up systems that program cuts can weaken.. In other words. a new prevention technology may arrive. but without a delivery network strong enough to reach people at highest risk. its public-health impact can stall.
There is also an accountability and transparency issue that public-health officials routinely rely on.. Over time, PEPFAR’s granular reporting has helped countries identify gaps early and adjust quickly.. The new reporting approach described in the data release—covering only select metrics and making some previously required reporting optional—could make it harder to see where the system is failing.. That matters because prevention shortfalls don’t always show up immediately in treatment numbers.. They can instead surface later as rising infections, strained facilities, and a delayed “hidden crisis” effect.
From a policy standpoint. the emerging pattern raises a hard question for HIV strategy in the years ahead: can a program claim success by holding treatment steady while allowing testing and prevention to erode?. For families and communities, the answer isn’t abstract.. It affects whether people get diagnosed in time. whether those at risk can access preventive options consistently. and whether health systems can keep pace with demand when outreach networks weaken.
For the United States, the political debate over foreign aid is also a debate about what outcomes count.. If the emphasis remains on topline treatment continuity alone, prevention gaps may widen quietly.. But if the data show that testing. PrEP. and prevention programs drop significantly after major administrative disruptions. then the longer-term costs—medical. economic. and human—could outlast any single quarter’s reassuring figures.
