PCOS might affect men too—what a name shift could mean
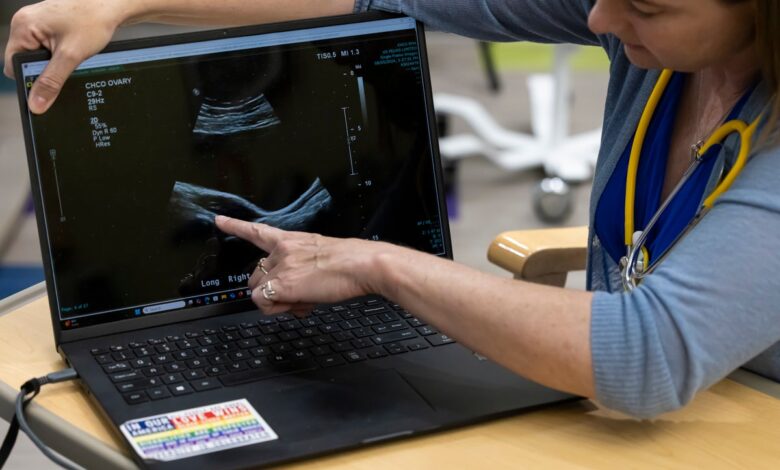
PCOS in – Research increasingly links PCOS biology to metabolic and hormonal risk in men—pushing experts to rethink the name and improve diagnosis and treatments for all.
PCOS has long been treated as a condition centered on ovaries, but Misryoum’s latest reporting shows the story may be bigger—and messier—than the name suggests.
Why PCOS’s “cysts” label never fit
Misryoum notes that when the condition was first described in the 1930s. physicians Stein and Leventhal identified enlarged ovaries and cycles that didn’t behave normally.. The fluid-filled structures they saw were labeled as cysts.. But modern understanding reframes those structures: they’re actually follicles—undeveloped egg-containing structures that resemble a “string of pearls” on today’s ultrasounds.. They don’t behave like true cysts, and they don’t rupture.
That matters because names can shape how medicine thinks. When clinicians view PCOS as a problem of cyst-like ovarian changes, the focus can drift away from the underlying metabolic and hormonal drivers that researchers believe are central.
A metabolic chain reaction—and evidence in families
In people with ovaries, one well-studied pathway starts with an inherited susceptibility that increases the risk of insulin resistance.. Insulin is produced by the pancreas and helps move glucose from the bloodstream into cells.. When insulin signaling doesn’t work properly, the body compensates by producing more insulin.. That elevated insulin environment can then encourage the ovaries to produce excess androgens such as testosterone. disrupting normal follicle development and ovulation.. The downstream results—irregular menstrual cycles and related symptoms—follow.
Azziz and Dunaif’s work, as described through Misryoum’s reporting, also points to the importance of family clustering.. When scientists examined relatives of people with PCOS. they found higher risks among siblings. raising the question that has become impossible to ignore: if PCOS risk travels through genes and metabolism. could men show parts of the same biology?
What men might share: weight. metabolic syndrome. hormone signals
In studies described by Misryoum. men showed increased odds of being overweight and having metabolic syndrome. a cluster of conditions that includes issues like insulin resistance. elevated blood pressure. and abnormal blood lipids.. Some research also points to elevated levels of a male hormone produced by the adrenal glands in younger men.
This doesn’t mean men “have PCOS” in the same way as people with ovaries.. But it does suggest the syndrome’s biology may not be confined to reproductive organs.. The same genetic susceptibility that shapes insulin and androgen signaling in one group may contribute to metabolic and hormonal patterns in another.
For many families, this could be practical news: metabolic risk isn’t always recognized early, and symptoms that don’t fit a female reproductive template can be missed in men.
The diagnostic gap: awareness lags behind the science
Dunaif’s concern. reflected in Misryoum’s coverage. is that clinicians who should be alert to the condition—particularly in general internal medicine—may not be trained to look for it.. That can create a double failure: people who do not fit the classic “ovary-centered” presentation may not receive the right evaluation. and people who do fit it may have treatment plans that underemphasize the metabolic drivers.
The result is not just confusion—it can mean missed opportunities for earlier screening, lifestyle support, or medical interventions that target insulin resistance and cardiometabolic risk.
Why the name change is gaining momentum
Azziz and Dunaif discuss a coordinated but unofficial process around a new name—kept under wraps for now in the reporting.. Misryoum also notes that there was a previous effort in 2012 to rename PCOS as “metabolic reproductive syndrome,” abbreviated as MRS.. That proposal faced concerns that the acronym could still reinforce the female-focused framing.
This is where Misryoum sees the deeper logic: renaming can shift research priorities and clinical attention.. There’s a historical precedent in the way medical communities adopted the term “metabolic syndrome. ” previously known as “syndrome X” while mechanisms were less clear.. Once the language better reflected the biology, Misryoum’s reporting points to a surge of research momentum.
Treatments, funding, and the urgent need to think beyond ovaries
He also points to the scope of the problem, arguing that PCOS affects a substantial share of people with ovaries—commonly cited in the range of 10–15%—and potentially a similar proportion of men through overlapping metabolic features. If that is true, then the public health implications are huge.
Misryoum’s editorial angle is that a name shift could be more than symbolic.. When the condition’s framing better matches its mechanisms. it becomes easier to design research. build clinical awareness. and develop interventions that address the metabolic root rather than just treating downstream symptoms.
The broader question Misryoum leaves readers with is simple: if PCOS biology can show up in men through metabolic and hormonal signals, why should diagnosis and treatment pathways remain locked to one organ system?
Whether the proposed renaming process succeeds or not, the research trajectory is clear in Misryoum’s reporting: PCOS is increasingly being understood as a metabolic-hormonal condition with implications that extend well beyond the ovaries.
